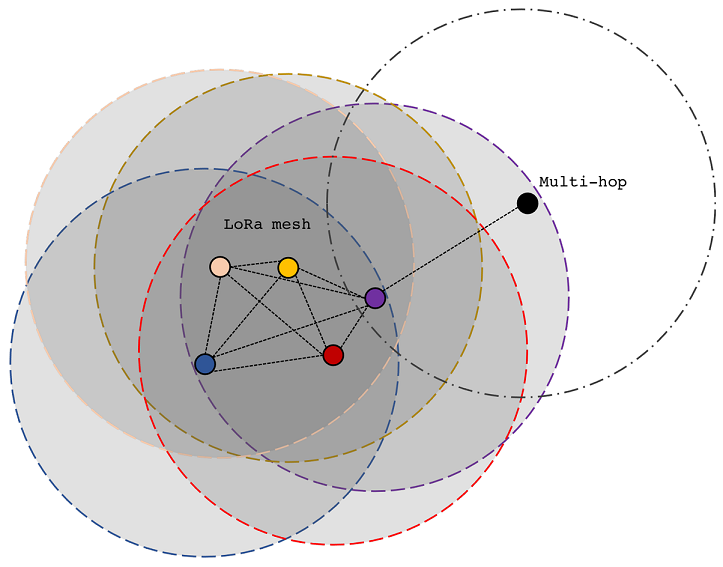
Giám sát IoT bằng Lora Mesh
Giới thiệu Lora Lora là công nghệ truyền không dây công suất thấp nhưng có thể truyền dữ liệu với khoảng cách lên đến hàng kilomet (km) mà không cần các thiết bị khuếch đại công suất.LoRa có thể được áp dụng trong các ứng dụng thu thập dữ liệu môi trường, trong đó mỗi …